Fiber Optic Probes: The Future of Liver Cancer Diagnosis
Insights | 08-02-2023 | By Liam Critchley
The bile duct is a key channel within the liver but is susceptible to becoming cancerous and is the second most common primary liver cancer. Most diagnoses of bile duct cancer come when it’s at an advanced stage and often too late, leading to poor survival rates. There are a number of techniques used to screen for bile duct cancer, such as radiological imaging and endoscopic procedures, however, they have some accuracy issues around distinguishing between cancerous and healthy bile ducts and insufficient sampling, respectively.
Therefore, new approaches are being sought that can detect any anomalies at the pre-cancerous stage and offer an early warning detection for bile duct cancer before it progresses to the later stages, where it is often incurable. Researchers are now looking towards optical methods for diagnosing bile duct cancer, with the latest piece of research focusing on an endoscopic optical light scattering technique.
Challenges of Bile Duct Cancer
Bile duct cancer, also known as cholangiocarcinoma, is often diagnosed at a late stage because people have no identifiable risk factor, resulting in fewer people that can be treated and higher mortality rates. Regarding treatment options, the only feasible options are for those with early-stage cholangiocarcinoma because they are surgery or transplant-based.
For a transplant or surgery to occur, the procedure is only performed if the cancer cells haven’t been transported away from the liver to other areas of the body―and in the later stages, the cells have already migrated, making early detection an important research area. Even if caught at an early cancerous stage and surgery is performed, the typical survival period is still only around 2 years post-surgery, so it’s important to actually diagnose it at the pre-cancer stage and before it’s taken hold in the liver any major way to not only ensure a higher chance of survival, but also a prolonged life after treatment.
However, this has typically proved challenging because it has an asymptomatic character and is located in an anatomically hard-to-access location. Despite the natural challenges, there have also been some technological challenges as well, with most diagnostic imaging methods used having a low specificity. As it stands, radiological images―such as ultrasound, X-ray computed tomography (CT), magnetic resonance cholangiopancreatography (MRCP), and positron emission tomography–computed tomography (PET-CT)―are used for the diagnosis, but their accuracy is a problem.
Moving Towards Optical Detection Methods
The inherent sensitivity and accuracy challenges with the status quo imaging methods have led to new analytical fields being explored, and optical detection methods have started to gather a lot of interest. One example has been to use narrow band imaging (NBI) at the haemoglobin absorption level to improve the visualisation of the mucosa during endoscopic approaches―such as probe-based confocal laser endomicroscopy (pCLE). While this approach has improved the detection of cancer lesions, the interpretation of the images is a complex process.
Another example that has emerged is to use of optical coherence tomography (OCT), which uses low-coherence near-infrared light to visualise the cross-sectional structure of mucosa. The use of OCT in both in-vivo and ex-vivo approaches has improved detection rates but is still unable to directly determine the abnormal cells and requires a considerable amount of training to use.
Given the progress so far, but still the relative challenges, researchers are starting to explore other optical-based methods to eliminate the diagnostic challenges associated with bile duct cancer detection, with fibre-optic label-free light scattering and absorption-based optical spectroscopic approaches now being explored.
Using Light Scattering to Build Detection Probes
Fibre-optic label-free light scattering and absorption-based optical spectroscopic methods encompass a range of techniques, including diffuse reflectance spectroscopy (DRS), elastic scattering spectroscopy (ESS), and light scattering spectroscopy (LSS). All these methods have advantages when it comes to imaging highly constrained spaces (like the bile duct) in-vivo.
These light scattering approaches are seen as promising because they can be made compatible with the smallest of catheters, don’t require an operator, require no exogenous markers, and allow for a quick investigation of large areas of tissue epithelial lining―which can then be used to detect any structural or biochemical changes in the tissue, including the presence of abnormal cells that could indicate cancer. LSS has already been used in this regard to probe the oesophagus and pancreas in pre-cancer screening approaches.
Researchers have now combined LSS and DRS imaging methods to adapt the imaging process for bile ducts. This has been achieved by constructing an inexpensive miniature LSS-DRS spatial gating fibre optic probe that is compatible with some minimally invasive in-vivo methods, including the small working channels of clinical cholangioscopes and ERCP catheters. This approach enabled the researchers to accurately investigate the internal cellular composition of the bile duct and detect any malignant transformations―with the LSS determining the cellular composition of the bile duct epithelium and DRS deducing the phenotypic properties of the underlying connective tissue.
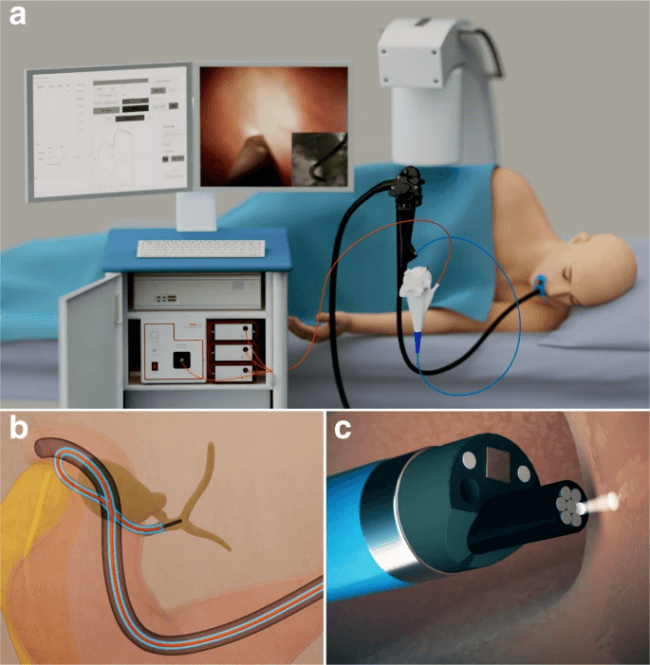
a An illustration depicting LSS-DRS measurements of the bile duct wall with the endoscopic light scattering spectroscopy system. A patient is positioned on an X-ray table, and a duodenoscope with a cholangioscope placed inside the duodenoscope working channel is inserted into the duodenum. The miniature LSS-DRS fiber optic probe with the delivery fiber coupled to a broadband xenon light source and collection fibers coupled to three spectrometers is inserted into the working channel of a cholangioscope. b The LSS-DRS fiber optic probe is passed into the pancreaticobiliary system. c The probe illuminates a location of the internal bile duct epithelial lining, and the spectra are acquired automatically when the probe is in close proximity to the bile duct wall.
This new approach was trialled on 29 patients who were undergoing routine ERCP procedures, with 13 being performed with ERCP catheters and 16 being performed with cholangioscopes. The choice of the ERCP technique was down to the individual clinician, which is why there was not the same amount of testing for both methods, but the results showed that the decision to choose one method over the other did not have any negative effect on the spectroscopic measurements.
No special training was needed to be given to the clinicians as the system operated automatically during the procedure and collected data without human input. During the study, this approach detected morphological changes in the epithelium, identifying any malignant transformations that would suggest that a patient has a bile duct pre-cancer or cancer. The approach was done with 97% accuracy, and the measurements were done in less than 2 minutes, so an optical spectroscopic approach could help better identify bile duct cancer early in its development using normal endoscopy procedures.
References:

